Posted on: 2 April 2026
Gail Mills has been the Health and Care Director (Nursing, Midwifery and Allied Health Professionals) for the NIHR Yorkshire and Humber Regional Research Delivery Network since 2024. Gail is also Associate Nurse Director for Research and Development at Sheffield Teaching Hospitals NHS Foundation Trust. Gail represents clinical research nursing nationally as Deputy Chair and Secretary for the RCN Clinical Research Nurse sub-committee and is the Deputy Lead for Workforce Development at the UK Clinical Research Facility Network (UKCRFN).

Hello, my name is Gail, and I’m part of the NIHR Research Delivery Network (RDN) in Yorkshire and Humber. My role provides leadership for research delivery and career development for health and care professionals including nurses, midwives and allied health professionals (AHPs) in the region.
Research, including world-leading studies and trials taking place here in our communities, plays an everyday role in all that we do in health and social care, and is only made possible by our wonderful research workforce. Within our region, hundreds of health and care staff play a crucial role in research delivery – working across a wide range of settings.
Without the power of health and care research, new treatments and preventative medicine and care wouldn’t be possible. Our Yorkshire and Humber research community is at the forefront of this - from preventative use of AI for a heart condition, ensuring children and young people understand the power of health and care research in mental health, and new treatments for flu. We’ve been proud to support these studies - and many more - within the NIHR RDN in Yorkshire and Humber.
2026 marks an important year for NIHR as we reflect on 20 years of supporting world-leading research and training for health and care professionals. As we celebrate two decades of impact – providing training, supporting research leaders and empowering a research-ready workforce – now is the time to explore how NIHR can support the next step in your career.
The NIHR funds or part-funds over 10,000 frontline research delivery staff across the NHS and wider health and care system. This includes research-specific roles, but also those who embed research into their everyday work - an important and rewarding step to begin your path in research.
As we celebrate such a significant milestone and reflect on our research workforce, I wanted to share just a handful of ways health and care staff in Yorkshire and Humber and beyond can begin or support their research journey.
- Kickstart or develop your research journey with NIHR opportunities: A key commitment of the RDN is to develop an internationally renowned, responsive, sustainable and diverse research delivery workforce. Via the NIHR website, you’ll find a range of programmes, study opportunities, funding and bespoke support to your profession in order to support this aim.
- Upskill or develop your knowledge via NIHR Learn: NIHR Learn is free-to-access for anyone – all you need is an email address. Discover learning programmes such as Good Clinical Practice (GCP) and refresh your knowledge or find out more ahead of key changes to GCP regulations from this month.
- Develop as a research leader with an NIHR-funded programme: Designed for nurses, midwives and AHPs, the NIHR’s Developing Research Leaders (DRL) Programme is a funded opportunity to build your research leadership skills and confidence, amongst other things. The programme closes to applications on 21 April 2026.
- Masters for Research Delivery Leadership: The Masters for Research Delivery Leadership (MRDL) is designed for experienced health and care professionals from all registered professional backgrounds who are looking to step into leadership roles in research delivery. Registered health and care professionals can apply for up to three years of funding to complete a postgraduate certificate, postgraduate diploma or master’s degree aligned with the MRDL.
- Add your study to Be Part of Research or share it with your patients: Health research needs all of us. Thousands of studies take place across the UK every year. Be Part of Research makes it easier for you to help your patients access and take part in research.
I’m proud to be part of the diverse and active research community we have in our region, who consistently deliver world-leading research which changes, improves and saves lives in our communities.
Thank you for reading.
The NIHR Research Delivery Network (RDN) is funded by the Department of Health and Social Care (DHSC), to enable the health and care system to attract, optimise and deliver research across England. The RDN supports health and care organisations across England to deliver research in hospitals, primary care and community and residential settings.
We also have a blog from Caroline Robinson, Senior Project Manager, NHS West Yorkshire Integrated Care Board (ICB), Cathi Ridding, Vocational Rehabilitation Clinical Lead and Abi Crabtree, Vocational Rehabilitation Clinical Lead, Bradford District and Craven Multi-system Rehabilitation Service

Hello, our names are Caroline, Abi and Cathi
In March, we launched the workplace long-term conditions guide. The guide encourages employees and employers to talk openly about health and aims to support them in making simple adjustments together, so everyone has the best chance to succeed at work. It has been a collaboration between the University of Aberdeen Business School, Bradford District and Craven Multi-system Rehabilitation Service and NHS West Yorkshire Integrated Care Board
Why do we need this guide?
Throughout our clinical careers in the NHS, we have witnessed the impact health has on a person’s ability to work. Not being in work can affect someone’s self-esteem, shatter their confidence and have an impact on a person’s physical and mental health. It can affect the health of the people around them whom they care for.
In the UK, over one in five people of working age are out of work and not looking for work. It has been estimated that 600,000 more people could leave work by 2030 due to ill health. In addition, economic inactivity caused by ill-health is estimated to cost the UK £212 billion annually. In West Yorkshire, the position is unfortunately higher than the national average. 26.3% of our working-age population is economically inactive compared to 21.6% nationally, or 19% excluding students, compared to 16% nationally.
These figures demonstrate the work that still needs to be done to help people secure and remain in work. This matters to us all because illness does not discriminate; yes, you can try and mitigate some of the risks of getting ill or having an accident, but it can happen to any one of us in our lifetimes.
 How does the guide help?
How does the guide help?
The guide is a tool to help improve the working environment. We know the working environment has an impact on health and wellbeing. Good working environments that are supportive and inclusive are good for employees and protective of health. They are also good for employers. Employees who are healthier are more engaged and more productive; they boost organisational performance. Working environments where people do not feel in control, experience high levels of stress, and have low levels of physical movement can worsen health.
One way to improve the working environment is through supportive relationships and honest discussion, which can feel difficult to achieve, but this guide will help. Employees may worry about the impact discussing their health could have on their career prospects, along with the stigma and discrimination they may face. Employers may be concerned about doing the wrong thing and worry that raising health issues may lead to unintended challenging situations. Sometimes, it may be that both employers and employees are not sure how to start the conversation. This guide helps make this easier by providing simple tools to encourage open discussions about health.
The guide also helps by suggesting reasonable adjustments which are linked to symptoms. This makes it easier for employees and employers to create an action plan together. Everyone has the right to get support at work. Supporting people at work is not about giving some people ‘special treatment’. It is about making sure everyone has the best chance to do well at their job, and by doing this, everyone benefits.
What else has been happening?
ICB leadership changes
As we have previously shared with you, ICB chief executive Rob Webster CBE will be leaving the organisation on 15 April, and Jonathan Webb, currently the ICB’s director of finance, will take over as interim chief executive. To support this arrangement, following an internal competitive interview process, Ian Currell has been appointed into the role of interim director of finance. This arrangement will continue until the new substantive chief executive is in post. Ian has worked in a number of senior finance roles across the NHS over many years and has significant senior leadership experience. Having Ian in this role will ensure both continuity and stability for the ICB, now and in the months ahead.

Sayma Mirza and Debi Gibson have been appointed to interim director of nursing positions, also following an internal recruitment exercise. Together with Ian Bennett, they will provide strong, collaborative leadership for our nursing function during this period of transition.
The team will work collaboratively across our functions, providing support to our West Yorkshire places, ensuring continuity and stability for the nursing directorate and the wider ICB in the months ahead. Sayma will cover Bradford District and Craven, Debi will cover Calderdale, Kirklees and Wakefield and Ian will cover Leeds.
Ian, Sayma and Debi will continue to champion our approach to partnership working and maintaining strong relationships as we move into new ways of working.
Julie Clennell will continue in her role as executive director of nursing until June 2026, adding additional stability during this period of transition.
CQC rates leadership at Bradford Teaching Hospitals NHS Foundation Trust as good
The Care Quality Commission (CQC) has rated Bradford Teaching Hospitals NHS Foundation Trust as good for how well-led it is following an inspection in November. You can read the report on the CQC website.
New all-age 24/7 mental health crisis text support service
 A new all-age 24/7 mental health crisis text support service launched this week (1 April), delivered by Mental Health Innovations (provider of SHOUT).
A new all-age 24/7 mental health crisis text support service launched this week (1 April), delivered by Mental Health Innovations (provider of SHOUT).
The delivery of an all-age crisis text service is a national NHSE ambition but is also important in ensuring that we improve accessibility to support during a crisis. Local and national insight shows that text is a preferred crisis offer for lots of people, including those who may have a neurodiversity, younger people or anyone who would prefer to communicate via text.
To use this free, confidential service, text BRIGHT to 85258.
Celebrating two years of being the first Keep it Local ICB and ICS in the country: National report on our trailblazing approach
 In March 2024, West Yorkshire became the first integrated care board (ICB) in the country to adopt Locality’s Keep it Local approach. With the five local authorities already signed up, this made West Yorkshire the first “Keep it Local” integrated care system (ICS); a commitment to prioritising working with, commissioning and supporting our local VCSE sector.
In March 2024, West Yorkshire became the first integrated care board (ICB) in the country to adopt Locality’s Keep it Local approach. With the five local authorities already signed up, this made West Yorkshire the first “Keep it Local” integrated care system (ICS); a commitment to prioritising working with, commissioning and supporting our local VCSE sector.
Following this, Locality worked with the Power of Communities (our strategic VCSE Alliance) to support its development and implementation of the approach in key areas as well as NHS West Yorkshire ICB winning Locality’s 2024 Keep it Local Award.
Locality have now launched their report on ‘How West Yorkshire became the first “Keep it Local” Integrated Care System’ sharing what health systems across the country can learn from our trailblazing approach to delivering a more prevention-focussed and neighbourhood-based health service grounded in our local VCSE organisations. It is also being launched alongside their report on ‘Keep it Local Health Commissioning Guide’ which has been shaped by our approach in West Yorkshire.
Inspirational video encourages cancer conversations about the importance of exercise
Physical exercise and simply moving around can have a hugely positive impact on patient experience and outcomes for people affected by cancer.West Yorkshire and Harrogate Cancer Alliance has partnered with Professor Shaunna Burke - Associate Professor in Exercise and Health Psychology in Leeds and an Everest summiteer - to produce this inspirational video, encouraging clinical teams to discuss the importance of exercise with their patients.
The video includes a QR code for clinicians to access training that can help them to have those conversations and improve the quality of life for people living with and beyond cancer. Watch on the WY Health and Care Partnership YouTube channel. Visit the Cancer Alliance website to view the video and access more resources for professionals supporting people living with and beyond cancer.
Asthma and COPD patients in West Yorkshire to receive better care closer to home
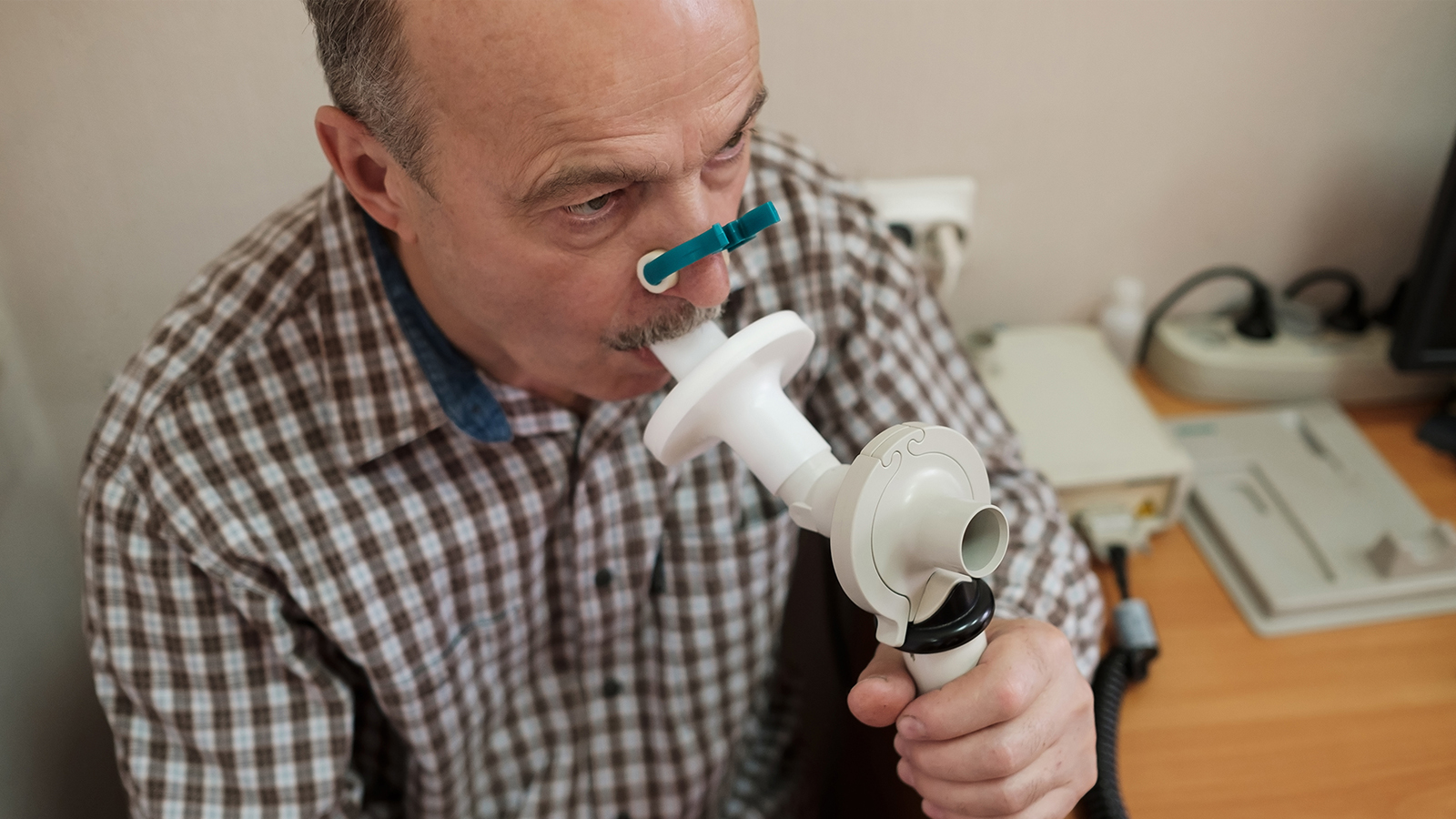 The Respiratory Transformation Partnership (RTP) aims to make better use of innovative treatments and technology. It brings together health innovation networks like Health Innovation Yorkshire and Humber alongside NHS organisations, industry, the Office for Life Sciences, NHS England and others to find and treat people who may not realise they have life-limiting conditions.
The Respiratory Transformation Partnership (RTP) aims to make better use of innovative treatments and technology. It brings together health innovation networks like Health Innovation Yorkshire and Humber alongside NHS organisations, industry, the Office for Life Sciences, NHS England and others to find and treat people who may not realise they have life-limiting conditions.
Health Innovation Yorkshire and Humber is working with the NHS West Yorkshire Integrated Care Board, Conexus Healthcare and Mid Yorkshire Teaching NHS Trust to improve care for patients with asthma and COPD.
One project in Wakefield has already begun analysing patient records across 34 GP practices to identify people who might have undiagnosed COPD or asthma. Since last October, practices have reviewed 1,233 patients, carried out 161 diagnostic spirometry tests and diagnosed 55 new cases of COPD and 14 new cases of asthma. Find out more on the Health Innovation website.
Working together to improve housing and health
Good quality housing is essential for good health. Preventing and responding to housing-related health issues requires co-ordinated working across housing, health and the voluntary sector. Our latest case study shows how we work together to make sure that effective practice in health and housing is routinely shared and to support opportunities to integrate services where we can. By doing this, we aim to help colleagues identify housing-related health risks earlier and respond more effectively. Read more on the Partnership website.
Adversity, Trauma and Resilience Awards - Five years. One night. Your stories.
 Leaders, practitioners and community organisations from across West Yorkshire came together at the Royal Armouries in Leeds on Monday 23 March to celebrate the Adversity, Trauma and Resilience Awards 2026. This landmark event marked five years of the West Yorkshire Adversity, Trauma and Resilience Programme. Hosted by journalist and broadcaster Tanya Arnold, the evening recognised the people and partnerships driving trauma-informed change across services, communities and systems.
Leaders, practitioners and community organisations from across West Yorkshire came together at the Royal Armouries in Leeds on Monday 23 March to celebrate the Adversity, Trauma and Resilience Awards 2026. This landmark event marked five years of the West Yorkshire Adversity, Trauma and Resilience Programme. Hosted by journalist and broadcaster Tanya Arnold, the evening recognised the people and partnerships driving trauma-informed change across services, communities and systems.
We received over 60 nominations across 12 award categories, highlighting the compassion, innovation and collaboration taking place across health, local authorities, education, policing, criminal justice and the voluntary, community and social enterprise sector. The awards celebrated individuals and teams who are helping create safer, more compassionate and more equitable systems for people affected by adversity and trauma. Congratulations to all award winners and nominees. Read more on the Partnership website news pages.
Stay well this Easter - plan ahead and help the NHS
With the Easter bank holidays approaching, the NHS in West Yorkshire is reminding people to get prepared as services are expected to be busy. Most GP practices and some pharmacies will close or may have different opening hours. Hospitals across the country continue to be busy but by planning ahead you’ll help keep services available for those who need them most.
There are two bank holidays coming up on 3 and 6 April. On these days, appointments with GPs and other healthcare professionals will still be available for urgent issues but this may not be at your usual GP practice. Appointments must be pre-booked by calling your own GP practice or by using NHS 111 online or calling 111. Read more on the Partnership website.
Resident doctors in England to go on strike this month
The British Medical Association (BMA) has confirmed that resident doctors will take industrial action from Tuesday 7 to Monday 13 April. Please see this news item Get the help you need during the resident doctors’ strike for more information.

